Persistent Pain
Persistent Pain Explained
Persistent pain (sometimes called chronic or long-term pain) is described as 'pain that continues for three months or more and may not respond to standard medical treatment'.
It can be debilitating and frustrating to manage and can also affect your relationships with family, friends and work colleagues.
The good news is there is usually lots you can do to help improve your quality of life.

What is persistent pain
Pain starts as an unpleasant signal in the body – think of it as a warning sign. It is designed to grab our attention and keeps going until we sort the problem out. To sum up:
- Pain demands our attention
- Pain demands an explanation
- Pain demands we get help
This is called a 'threat' response, so our brain downloads chemicals to make sure we take action:
- muscle tension and protective chemicals to guard against further damage
- worry and anxiety chemicals to find out what is wrong
- stress chemicals to make us respond and get help
Persistent pain is triggered when the nerves carrying unpleasant information become irritated and continue to react even though the initial cause has healed. Sometimes the pain system stays switched on, perhaps after surgery or changes in posture. The threat chemicals continue to download, making the system fire again - this is known as the vicious cycle of pain.
Your nervous system may be wary of anything that makes it react – activity, inactivity, changes in weather, or even unpredictable triggers.
Pain management is about helping the body produce chemicals to make a threatened system feel safer.
Acceptance
Acceptance is not about giving up, but accepting that the pain will remain with you and is not curable can certainly be a challenge.
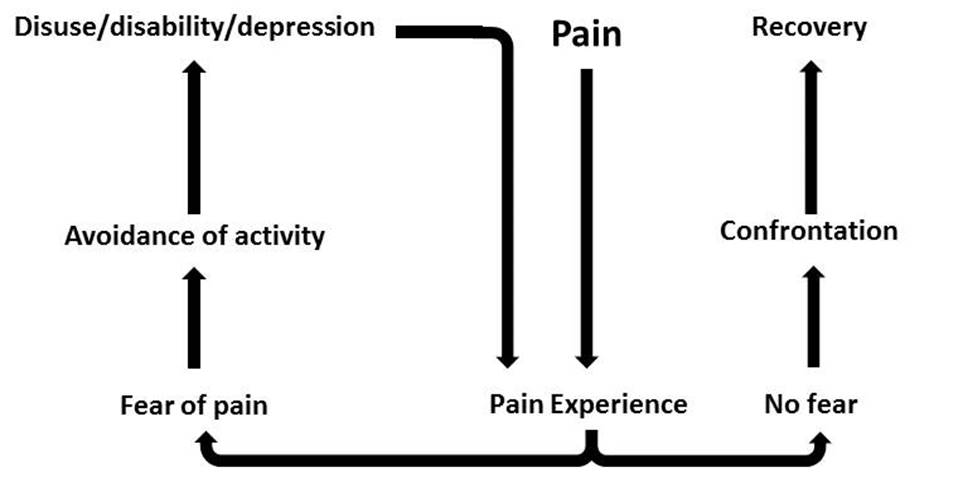
Persistent pain is a bit like an unwanted visitor that can keep some people searching for possible treatments to keep their unwelcome guest away. The stress of focusing on the pain itself only makes the suffering much worse.
Although some people understand this straight away, acceptance can happen over time. You will become more accepting as you take action to focus on goals and the way you want your life to be.
It’s not about focusing repeatedly on a life spent trying to get rid of the pain. Accepting changes and losses can take time, but sharing these issues with someone you trust can be helpful. Recognising unexpected positives like meeting new people and doing different things in new ways can provide a real boost.
Being patient with and kind to yourself also makes a real difference, rather than worrying about the negatives in life caused by pain.
Improving Pain
Sadly, medications can’t cure persistent pain. They can only lessen it by 40%, at best, and often by less.
If drugs don’t provide the relief you expected, it can lead to frustration and worry. This, in turn, adds to the stress of pain and a vicious cycle sets in.
To get the best out of the medication your GP has prescribed it’s important you:
- Use the correct doses and right timings
- Don't wait until pain levels are severe before using medication
- Discuss reducing usage with your GP before cutting down over time or stopping
Managing pain without medication
GETTING FITTER
For most people living with persistent pain, staying fit and active can be a real challenge. Often the natural reaction to pain is to want to rest and avoid too much movement.
People with pain and health care professionals now know that one of the main ways to live a better quality of life is to get fitter. This helps strengthen your muscles and increases flexibility in your joints. Becoming fitter will help you slowly build more energy and have better sleep patterns.
The way most people with pain get fitter is to slowly increase the level of activities and set themselves fun goals. Pacing is a skill which will help you become more active and stay active - without increasing pain or tiredness.

It is important to remember that more pain does not always mean you are doing damage to your body. It may mean you are stretching muscles and nerves that are stiff and tight which is a ‘normal’ pain.
Most importantly, find something that you enjoy. It often helps to do activities with friends. Make sure you have fun and it will be a lot easier!
Goal setting
Goals can be focused on any aspect of daily life including
- Feel better about yourself
- Have more energy
- Be more confident in coping
- Help reduce and manage your pain better
This may help develop goals and encourage a can do attitude even over small tasks. It is important these goals are achievable so as not to diminish confidence and affect your mood. Begin with simple daily tasks and gradually build up, discuss your planned goals with your health professional if you are struggling and consider planning and prioritising.
An Action plan may help prioritise activities that:
- must be done today
- might be done in the next few days
- need not be done at all or could be done by others
It is important here to consider your personality type.
To make it easy to remember use the SMART goal formula:
S= specific activity (something active and enjoyable)
M= measureable (how far you or how long or how often you have done the activity)
A= achievable (can do it everyday at chosen time)
R= realistic (possible to do in time and place where you are)
T= time bound (set time for length of activity to reduce unhelpful over-doing or under-doing the activity)
Build up slowly and steadily. When the activity becomes very easy to do, increase the time or distance. You can make a new activity goal or choose to maintain the same activity every day. It can help to find activity programmes in your area to help you start and keep going.
Planning and Pacing
Pain can affect how you manage the range of activities in your day. We can tend to use pain as a guide: "Oh, my pain has increased…I’d better stop or rest." Or: "I must get this done before the pain increases again."
Sound familiar? It’s very common to fall into an unhelpful trap of over-doing or ‘trying to keep up’ patterns, where on days with less pain you find yourself doing catch-up jobs, extra work and spending more time to complete the task or activity.
Sometimes only pain or tiredness stops you. Then you find you have severe pain flare-ups, are exhausted and have to rest for hours or days until pain levels lessen. This pattern is called the ‘Boom and Bust cycle’.
It leads to being stuck in the vicious cycle of pain. It is miserable and your confidence drops. Taking action early to plan in a more balanced approach means less severe pain flare-ups which impact on your health and life.
Learning to find your personal balance of activity and relaxation – such as changing or doing activities in different postures and places - can lead to a better life. Building confidence like this means you can do more of the things you want.
Assessing your progress
Being aware of your pain and measuring how you are managing it is an important part of coping well. Understanding when you are having a good or bad day can help you to pace your activities and avoid flare-ups.
Try the pain confidence test to help identify your current needs in managing your pain. This simple, 3-step questionnaire is an easy way to check on confidence levels to cope with life despite the pain. It will help you to think about the issues affecting you and enable you to plan how to deal with them. You can also use it to track your progress every week or two.
If you find you are struggling, this may mean you need more support and help from your health professional and your friends and family. Consider why this may be, there are strong links to persistent pain effecting sleep patterns and mood which will have negative impacts on your progress, do you need help with these aspects of your pain management rather than the completion of functional tasks?


